Unraveling the Unexpected Twist in Postoperative Wound Care
The world of modern medicine is full of surprises. Wound care, particularly after surgical procedures like total knee arthroplasty (TKA), has long been considered routine. However, even in such well-established practices, there are tricky parts and tangled issues that can catch providers off guard. One such example is the unexpected allergic reaction to silver sulfate present in wound dressings. In this opinion editorial, we take a closer look at these perplexing events and share insights based on one unusual case, all while offering a balanced perspective that is both neutral and informative.
When patients undergo a procedure as common as TKA, they expect not only successful joint replacement but also a smooth path to recovery. As surgeons and wound care teams work together to protect the surgical site, the use of silver-based dressings has become a super important part of the strategy to ward off infections. Yet, as the story unfolds, we find that even trusted materials can sometimes produce confusing symptoms. This article will help you get into the little details behind such episodes and compare the benefits against the risks in daily clinical practice.
Silver-Based Dressings: Benefits and Unexpected Pitfalls
Silver-containing wound dressings have earned their place in the medical arena largely because of their anti-bacterial and anti-inflammatory properties. Their use is supported by numerous studies showing that they help fight off infections and promote proper healing in both surgical and traumatic wounds. Clinicians often appreciate these dressings for the edge they provide in managing complicated pieces like surgical site infections. However, as with many modern interventions, there is a flip side—a handful of cases where silver compounds trigger allergic reactions that are not immediately obvious.
To break down the scenario:
- Silver ions are released slowly over time, providing a continuous shield against bacteria.
- The dressing itself is made from advanced synthetic materials combined with silver sulfate to enhance its antimicrobial effects.
- For the vast majority of patients, these dressings work well and contribute to faster recovery times.
- However, a small subset of patients may have a hidden sensitivity to silver, leading to allergic contact dermatitis (ACD).
These bullet points illustrate the fine balance clinicians must maintain between harnessing the benefits of silver and being ready for the little twists that can turn a protective measure into a source of patient distress.
Case Study Spotlight: Allergic Reaction After Total Knee Arthroplasty
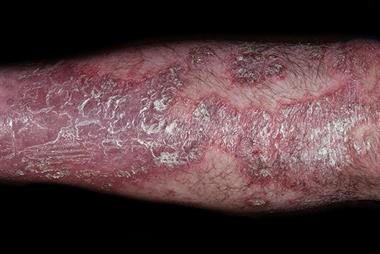
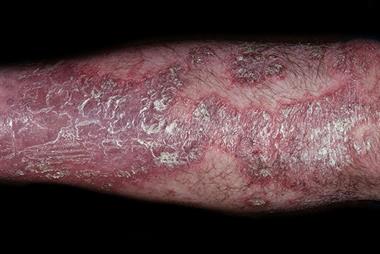
Let’s get into a case that has stirred discussions among healthcare professionals. A 55-year-old woman, with preexisting conditions like diabetes mellitus and hypertension, underwent TKA for advanced osteoarthritis. Her surgery was performed after her HbA1c levels were managed adequately—a key concern, given that diabetic wounds can be tricky to manage. What seemed like a standard postoperative regimen took an unexpected turn when she developed erythema, itching, and a burning sensation around her knee.
In this particular incident, the patient had her wound covered with a silver sulfate-containing dressing—a product marketed to optimize wound healing and protect against infection. However, over the course of a week, the reaction started to build up. The timing and presentation led clinicians to suspect an allergic response rather than an infection.
Dissecting the Telltale Signs of Allergic Contact Dermatitis
Allergic contact dermatitis is an immune-mediated reaction that can emerge after repeated exposure to an allergen. In our case, the silver ions, which are usually the heroes, turned into unexpected villains by binding with skin proteins and initiating a T-cell mediated response. Here are some subtle details that can help sort out an allergic reaction from other conditions like irritant contact dermatitis or a bacterial infection:
- Erythema and Edema: These symptoms are common to many skin irritations. But when they present alongside localized itching and burning, they demand a closer look.
- Localized Reaction: The inflammation was limited to the region where the dressing was applied. This is a key indicator that the problem is related to direct contact with an allergen.
- Timing: Unlike infections, which can escalate rapidly, allergic reactions often have a delayed onset. In our case, symptoms were noted several days post-application, aligning well with a classic delayed hypersensitivity response.
Clinicians confirmed the diagnosis through patch testing, which showed a positive reaction to silver. This evidence was essential in ruling out other causes and helped guide the treatment plan toward managing ACD specifically.
Spotlight on Differential Diagnosis: Allergic vs. Irritant Contact Dermatitis
One of the challenges faced by health professionals is distinguishing between allergic contact dermatitis and irritant contact dermatitis. Both conditions share certain presentation traits such as redness and swelling, but the underlying causes are quite different. While irritant contact dermatitis results from direct damage to the skin’s protective barrier by some chemical or physical factor, allergic contact dermatitis is an immune response triggered by an allergen.
To help figure out which is which, consider the following table that outlines these subtle differences:
| Characteristic | Allergic Contact Dermatitis (ACD) | Irritant Contact Dermatitis (ICD) |
|---|---|---|
| Cause | Immune-mediated reaction to an allergen | Direct toxic effect causing skin barrier damage |
| Onset | Delayed (24 to 72 hours or more) | Immediate or within a few hours of exposure |
| Distribution | Localized to the contact area; may spread due to immune response | Mostly confined to the area of contact |
| Symptoms | Itching, redness, burning, sometimes vesicles | Redness, dryness, cracking, and burning sensations |
This table illustrates the small distinctions in clinical presentation that require you to get into the nitty-gritty when diagnosing skin reactions. In our patient’s case, the delayed reaction alongside localized symptoms pointed directly towards allergic contact dermatitis, making a strong case for discontinuing the silver sulfate dressing.
Balancing Benefits and Risks in Wound Management
Silver-based products have long been hailed as a super important component in modern wound care. They are celebrated for their broad antimicrobial properties, which help reduce the risk of postoperative infections—a common worry in surgical practice. Yet, as seen from this unusual case, even well-tested interventions can sometimes backfire due to patient-specific sensitivities.
When discussing these scenarios, it’s essential to weigh the benefits against the risks. Here are some key considerations for clinicians:
- Patient History: A detailed medical history including prior exposures and known allergies remains essential. In many instances, allergies to metals like silver are not well-documented because exposure is limited.
- Close Monitoring: After applying advanced dressings, healthcare providers should monitor the patient closely for any signs that might indicate a developing allergic response.
- Alternative Options: Not all dressings contain silver. In patients suspected to be at risk, alternative wound care products that are free from silver or other heavy metals should be considered.
- Timely Intervention: Early recognition of adverse reactions can significantly reduce the risk of complications such as extended inflammation or secondary infections.
Clinicians need to figure a path through these challenging bits by having a robust strategy that includes proper patient education, thorough history taking, and, when necessary, the flexibility to switch to an alternative dressing quickly. This approach is especially critical when treating populations that may already be vulnerable—for instance, patients with diabetes, where even minor complications can quickly become full of problems.
Strategies for Managing Silver-Allergic Reactions in a Clinical Setting
Tackling an allergic reaction, especially one caused by something as unexpected as a silver-based dressing, can feel overwhelming. However, there are clear steps that can help sort out the situation and steer through the difficulties with a systematic approach. Here is an outline of some key management strategies:
- Immediate Removal: Once an allergic reaction is suspected, removing the offending agent is the first step. In our patient’s case, replacing the silver sulfate-containing dressing with a non-silver alternative was crucial.
- Symptom Relief: Administration of antihistamines (like loratadine) and topical corticosteroids or other soothing agents (such as dimetindene ointment) can help ease symptoms like itching and burning.
- Preventive Antibiotics: Especially in individuals with underlying conditions such as diabetes, a brief course of prophylactic antibiotics might be prescribed to ward off secondary infections.
- Follow-Up and Monitoring: Regular follow-up visits are critical for assessing wound healing and ensuring that the allergic response subsides. Recording improvements at intervals (for example, at 1, 2, 3, 4, and 12 weeks post-intervention) also provides valuable information.
- Patch Testing: Confirming the diagnosis with patch testing after the initial clinical assessment helps establish the precise allergen responsible and informs future treatment plans.
This systematic list not only highlights the steps required to manage the allergic reaction but also reinforces the importance of early diagnosis and effective patient management in preventing more serious complications. It also helps all stakeholders—clinicians, nurses, and patients—understand exactly what to expect and how to work together for the best outcomes.
Considerations for Diabetic Patients and Wound Care Decisions
Diabetic patients already walk a nerve-racking path when it comes to wound healing. Their wounds tend to be more prone to infections and other healing challenges. Adding the possibility of an allergic reaction to the mix can create an off-putting scenario where every decision matters. It is essential that healthcare providers take extra care when choosing wound dressings for patients with diabetes or other chronic conditions.
Some key points for these patients include:
- Detailed Medical Screening: Before selecting any dressing, a full assessment of the patient’s previous exposures and any potential allergies should be performed.
- Alternative Dressing Options: If silver-based products are suspected to trigger a reaction, providers may opt to use dressings that incorporate different antimicrobial agents.
- Frequent Monitoring: Given the heightened risk of complications, it is super important that diabetic patients are monitored very closely postoperatively.
- Patient Education: Informing patients about the signs and symptoms of allergic reactions empowers them to notify their healthcare providers quickly should any issues arise.
Comparing the benefits and risks and taking extra care in vulnerable groups is a key lesson taught by this case. The delicate balance between safeguarding against infections and avoiding allergic reactions demands that providers get around the maze of patient-specific issues with confidence and preparedness.
Exploring the Fine Points of Allergic Reactions to Metals
Silver is not the only metal that can trigger an allergic response. Metals like nickel, cobalt, and chromium also feature in various medical products. What sets silver apart is its broad use in dressings and topical applications, making it a common ingredient in the plethora of products designed to support wound healing. Yet, even this valuable metal can sometimes be a source of trouble.
The fine points of allergic reactions to metals can be better understood when we look at the underlying concept of metal hypersensitivity:
- The Immunologic Mechanism: The immune system may interpret metal ions as foreign invaders. When these ions bind to proteins in the skin, tiny complexes are formed that can trigger a T-cell response. This reaction takes time to build up and is often noticed only after repeated exposure.
- Subtle Patient Variability: Not all patients develop allergies to metals. It often depends on genetic predispositions and the level of exposure. For many, silver in small doses is harmless, while in others, even minimal exposure can lead to noticeable symptoms.
- Role of Patch Testing: Patch testing serves as the gold standard to identify which metal is responsible for an allergic reaction. It is a helpful tool that clinicians use to decide whether to continue with a particular wound dressing or opt for an alternative product.
Understanding these little twists in the allergic response process requires that healthcare providers dig into the hidden complexities of immune reactions. Awareness of such possibilities is crucial in modern clinical practice, where even a small adverse reaction can impact patient outcomes significantly.
How Clinicians Can Figure a Path Through Testing and Diagnosis
The journey from identifying a potential allergic reaction to confirming a diagnosis can be long and riddled with tension. However, there are ways to make your way through these challenges effectively. Let’s break down the common steps involved when clinicians face a suspected case of ACD due to silver exposure:
- Initial Clinical Evaluation: This involves asking patients detailed questions about their recent exposures, including the type of dressings used, timing of symptom onset, and history of similar reactions.
- Observation of the Reaction: Clinicians take note of the distribution of the rash and any associated symptoms like itching, redness, and burning. This observation is critical in forming a preliminary diagnosis.
- Patch Testing: Once inflammation is noted, a confirmatory patch test is usually performed. This test helps to pinpoint silver as the allergen and rule out other potential irritants.
- Follow-up Monitoring: After the diagnosis is made and treatment is initiated—often by switching to a non-silver dressing—regular follow-up visits are arranged to monitor healing and ensure that the allergic reaction resolves.
Understanding these small distinctions speeds up patient care and helps avoid future complications. For instance, if an allergy to silver is confirmed, that knowledge will drive the choice of dressing in subsequent procedures. Clearly outlining each step helps both new and experienced practitioners feel less intimidated by the process.
Essential Lessons for Future Practice
The case of allergic contact dermatitis from silver sulfate in a postoperative setting teaches us several super important lessons that can refine future medical practice. Let’s take a few moments to reflect on some actionable insights:
- Thorough History Taking Is Key:
- Ask detailed questions about past exposures to metals and wound dressings.
- Record any previous minor skin reactions, even if they were dismissed at the time.
- Flexibility in Treatment Choices:
- Be prepared with alternative dressings that do not contain metals if a patient is suspected of having a sensitivity.
- Keep informed about new developments in wound care products that offer similar antimicrobial benefits without using silver.
- Clear Communication and Education:
- Make sure that both the patient and the entire clinical team are aware of the signs that constitute an allergic reaction.
- Empower patients with knowledge so they can promptly report any unusual skin reactions or discomfort.
- Regular Reassessment:
- Schedule regular follow-up visits to monitor wound progress and address any lingering issues.
- Document every aspect of the patient’s response to the dressing to improve future care guidelines.
These lessons are especially useful for hospitals and outpatient settings where such experiences have a ripple effect on broader wound management practices. When every member of the clinical team keeps these key points in mind, the overall quality of patient care improves dramatically.
Expert Opinions on the Use of Silver in Wound Care
Opinions among healthcare professionals can sometimes be divided when it comes to silver-based wound dressings. While many acknowledge the critical antimicrobial benefits they offer, others stress the importance of not losing sight of potential allergic reactions. Here are some perspectives that showcase various viewpoints on this topic:
- Advocates of Silver Dressings:
Many surgeons and wound care specialists emphasize that silver dressings are essential in reducing the risk of postoperative infections. They argue that millions of patients have benefited from these products without any issues. For these experts, the key is to remain vigilant and manage the rare allergic reactions when they occur.
- Skeptical Voices:
On the other hand, some professionals are more cautious. They advocate for personalized patient care and highlight that even a small risk, particularly in sensitive populations like diabetics, warrants alternative products. For them, the choice of a silver dressing should always come with careful attention to patient history and readiness to intervene at the first sign of an allergic reaction.
- Balanced Approaches:
Most experts agree on a middle path: while silver dressings are undeniably useful, they should be one tool among many in a clinician’s wound care kit. Rather than discarding an effective product altogether, they propose advanced screening and prompt switching of dressings when necessary. This balanced approach helps maintain patient safety without sacrificing the antimicrobial benefits that silver provides.
By incorporating these expert insights into everyday practice, healthcare providers can better manage the tricky parts and tangled issues that sometimes arise in wound care. The collective experience in the field reinforces the idea that every treatment modality, no matter how routine it may seem, deserves careful scrutiny and a personalized approach.
Innovations and Future Directions in Wound Care Technology
The evolving field of wound care is continuously adapting to the fine points of patient needs. Innovations are on the horizon that aim to reduce the potential for allergic reactions while maintaining or even enhancing antimicrobial activity. Researchers are exploring several alternatives to traditional silver-based dressings, including:
- Nanotechnology-Based Solutions:
By using silver nanoparticles, manufacturers can potentially control the release of silver ions more precisely. This tactic might help reduce the quantity of silver that comes into direct contact with the skin, thus minimizing the likelihood of an allergic reaction.
- Bioengineered Dressings:
These dressings use materials derived from biological sources and are sometimes combined with antimicrobial peptides. They aim to mimic the natural healing environment while reducing the risk of allergic responses to synthetic metals.
- Customized Wound Care Protocols:
Personalized medicine is gradually making its way into wound care. By analyzing a patient’s genetic predispositions and prior exposure history, clinicians may eventually be able to predict who is more likely to experience an allergic reaction and adjust treatment plans accordingly.
While these innovations are still in various stages of research and clinical trials, they highlight the forward-thinking directions that the wound care industry is exploring. As new products emerge, they may solve some of the tricky parts associated with silver exposure while preserving the benefits that have made silver products so popular in the first place.
Turning a New Leaf: Patient Empowerment and Informed Decision-Making
One of the most significant lessons from the case of silver-induced allergic contact dermatitis is the importance of patient empowerment. When patients are well-informed about the potential side effects of any treatment, including something as seemingly straightforward as a wound dressing, they become active participants in protecting their own health.
Practical steps to enhance patient empowerment include:
- Advice and Information:
Clinicians should clearly articulate the benefits and possible side effects of using silver-based dressings. Providing written materials and guidelines can help patients recognize the early signs of an allergic reaction.
- Open Communication Channels:
Patients should be encouraged to report any unusual symptoms immediately. Establishing dedicated lines of communication or follow-up procedures can make a significant difference in early detection and timely intervention.
- Shared Decision-Making:
Involving patients in choosing their wound care products can help foster trust and ensure that care decisions are fully aligned with the patient’s comfort and safety levels.
By taking these steps, healthcare providers not only improve the immediate management of complications, but they also build a foundation for a more informed and cooperative doctor-patient relationship. This collaborative approach can make even nerve-racking situations easier to manage.
Final Thoughts: A Balanced View on Modern Wound Care
In conclusion, the case of allergic contact dermatitis triggered by silver sulfate in a post-TKA patient reminds us that the path to recovery is rarely straightforward. While silver-based dressings remain a key tool in our wound care arsenal, they come with their own set of twists and turns that merit careful attention. Healthcare providers must steer through these challenges by:
- Taking detailed patient histories
- Monitoring wound responses closely
- Remaining open to alternative treatment options
- Empowering patients with the right information
- Embracing innovations that could reduce risks
This balanced approach allows modern medicine to benefit from advanced technologies while acknowledging and managing the occasional pitfalls. When clinicians and patients work together, the hurdles—however intimidating they may appear—can be navigated with care and confidence.
The world of postoperative wound care is, indeed, full of little details and confusing bits that require ongoing attention. However, every challenge also presents an opportunity for improvement. As our collective knowledge grows, so too does our ability to craft personalized treatment plans that safeguard recovery while avoiding unnecessary complications.
Ultimately, while the risk of an allergic reaction to silver may remain low, understanding and preparing for such possibilities can transform a potentially nerve-racking experience into a manageable part of overall patient care. With careful monitoring, advanced screening, and a commitment to patient education, the benefits of silver and similar products can continue to be enjoyed safely.
Key Takeaways and Future Implications
To summarize the important points discussed in this editorial:
- Silver-based wound dressings offer essential antimicrobial benefits, yet even trusted methods can sometimes produce unexpected allergic responses.
- Differentiating between allergic and irritant contact dermatitis requires being mindful of confusing bits such as timing and localized symptoms.
- Clinicians must remain ready to change treatment approaches when signs of allergic contact dermatitis—like localized itching, redness, and burning—appear.
- A thorough patient history, especially in populations like diabetics, is key to preventing complications.
- Future advances in wound care may bring innovative products that minimize the risk of allergic reactions while preserving healing benefits.
These takeaways are not merely academic; they carry real-world implications that can influence guidelines, promote safer wound care protocols, and foster a more collaborative relationship between patients and their caregivers.
As the medical community continues to refine best practices and integrate new technology, the journey of treating surgical wounds will undoubtedly evolve. Staying aware of the tiny twists and turns along the way—while embracing innovation—can help ensure that our patients receive care that is both safe and effective.
Looking Ahead: Embracing a Future of Personalized Wound Care
Looking to the future, the intersection of modern technology and personalized medicine promises exciting new ways to manage wound care. Researchers are actively exploring methods that could one day allow for bespoke wound dressing solutions tailored to each individual patient’s needs.
Imagine a scenario where a preoperative screening can predict an individual’s likelihood of reacting to certain compounds, thereby guiding the choice of dressing. Such precision would not only eliminate unnecessary risks but also pave the way for more efficient recoveries. This prospect requires that all stakeholders—clinicians, researchers, manufacturers, and patients—work together to take a closer look at the small distinctions that can make or break a treatment regimen.
The continuing dialogue around cases like the silver sulfate-induced allergic contact dermatitis emphasizes the need for flexible, adaptive standards in modern medicine. As we learn from these cases, adjusting both practice guidelines and educational resources is essential. In turn, such improvements can create a safer, more predictable healing environment for patients who entrust their recovery to modern medical techniques.
Ultimately, the story behind this case serves as a reminder that in medicine, every innovation carries its own set of challenges. It is through acknowledging and addressing these challenges—by digging into the little details and being ready to adjust our approach—that we can continue to offer wound care solutions that uphold the highest standards of patient safety and efficacy.
While silver remains a powerful ally in reducing infection risk, its potential as an allergen should not be overlooked. With improved diagnostic methods, enhanced screening protocols, and a commitment to patient-centered care, the future of wound management looks promising, even as it demands our constant attention to the puzzling and the unexpected.
Conclusion: A Call for Vigilance and Collaboration in Wound Care
This opinion editorial has aimed to shine a light on the overlooked yet important topic of allergic contact dermatitis induced by silver-based wound dressings after total knee arthroplasty. The case discussed here is a reminder that even standard protocols come with hidden challenges. Through open dialogue, continuous research, and a willingness to adapt, we can effectively figure a path through these nerve-racking moments.
It is our hope that healthcare providers will use this information to better guide their clinical decisions, especially for patients with underlying conditions like diabetes that predispose them to complications. By staying informed, actively monitoring for early signs of allergic reactions, and being ready to replace a silver dressing with an alternative when necessary, patients can receive care that is both innovative and safe.
In the ever-evolving field of wound care, the ability to manage complications with poise and preparedness is indispensable. Every patient encounter offers an opportunity to learn, adapt, and improve the treatment pathways that define modern medicine. Let us embrace these learning moments and work together to ensure that every treatment decision reflects a true commitment to patient well-being.
Ultimately, balancing the benefits of advanced wound dressings with the need for vigilant monitoring can help shape a future where every recovery journey is as smooth as possible—even in the face of unexpected allergic reactions. It is through ongoing education, interdisciplinary collaboration, and patient-focused strategies that we will continue to refine our practices and enhance the overall quality of care.
Read more about this topic at
Metal Allergy to Surgical Plates, Screws, and Implants
Nickel allergy – Symptoms & causes